The Numbers & The Story
What is Healthy Start?
Healthy Start is a federal grant program aimed at improving health outcomes for women, infants, and their families. The program looks at many different health issues, but the overarching goal is to reduce infant mortality and maternal mortality.
What is Infant Mortality?
Infant mortality is the death of an infant before his or her first birthday. The infant mortality rate is based on the number of infant deaths for every 1,000 live births. In addition to giving us key information about maternal and infant health, the infant mortality rate is an important marker of the overall health of a society.
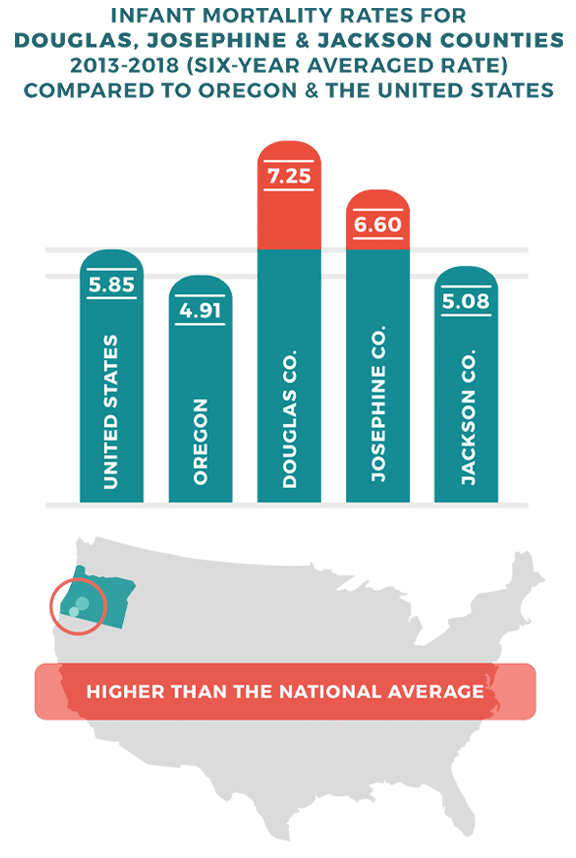
As a nation, our Infant Mortality Rate is just under 6 deaths per 1,000 live births; and for the state of Oregon, the rate is even lower.
Unfortunately, our region of Southern Oregon experiences higher rates of infant mortality: Josephine county at 6.60 and Douglas county at 7.25, based on six-year averages.
What is Maternal Mortality?
Maternal mortality, or pregnancy-related death, is defined as the death of a woman during pregnancy or within one year of the end of pregnancy from a pregnancy complication, a chain of events initiated by pregnancy, or the aggravation of an unrelated condition by the physiologic effects of pregnancy. The death of a woman during pregnancy, at delivery, or soon after delivery is a tragedy for her family and for society as a whole. Sadly, about 700 women die each year in the United States as a result of pregnancy or delivery complications.
Who is Impacted?
Communities of color are disproportionately affected by infant and maternal mortality. Black, American Indian, and Alaska Native women are two to three times more likely to die from pregnancy-related causes than white women – and this disparity increases with age.
In 2019, the national infant mortality rates by race and ethnicity were as follows:
- Non-Hispanic Black: 10.6
- Non-Hispanic Native Hawaiian or other Pacific Islander: 8.2
- Non-Hispanic American Indian/Alaska Native: 7.9
- Hispanic: 5.0
- Non-Hispanic white: 4.5
- Non-Hispanic Asian: 3.4
What’s the Cause?
Infant mortality and maternal mortality rates are not simply the result of personal health, family history, or accidents. These are complex health issues that are impacted by things like income, access to high-quality healthcare, affordable housing, family support, nutrition, community safety, availability of child care, exposure to pollutants, education, employment opportunities, and the many other parts of our lives that can have an impact on our health and well-being. These are “social determinants of health.”
What’s Happening in Southern Oregon?
There are significant racial and ethnic disparities in pregnancy and birth outcomes in the United States. Nationally, non-white mothers have higher rates of maternal mortality and morbidity, pre-term births, low birth weight, and infant mortalities. These same disparities are present in Southern Oregon.
Here are a few other key areas of community health we look at in Southern Oregon:
Food Security
Food security is defined by the U.S. Department of Agriculture as “access by all people at all times to enough food for an active, healthy life.” Over 15% of all residents in Douglas and Josephine Counties are food insecure, but this rate is higher for children with one in four children in our region being food insecure.

Unemployment
Our area’s unemployment rate continues to regularly exceed the state rate.
Poverty Status
Both Douglas and Josephine counties have higher poverty rates than Oregon and the U.S. Over one in four children in the region live in poverty.
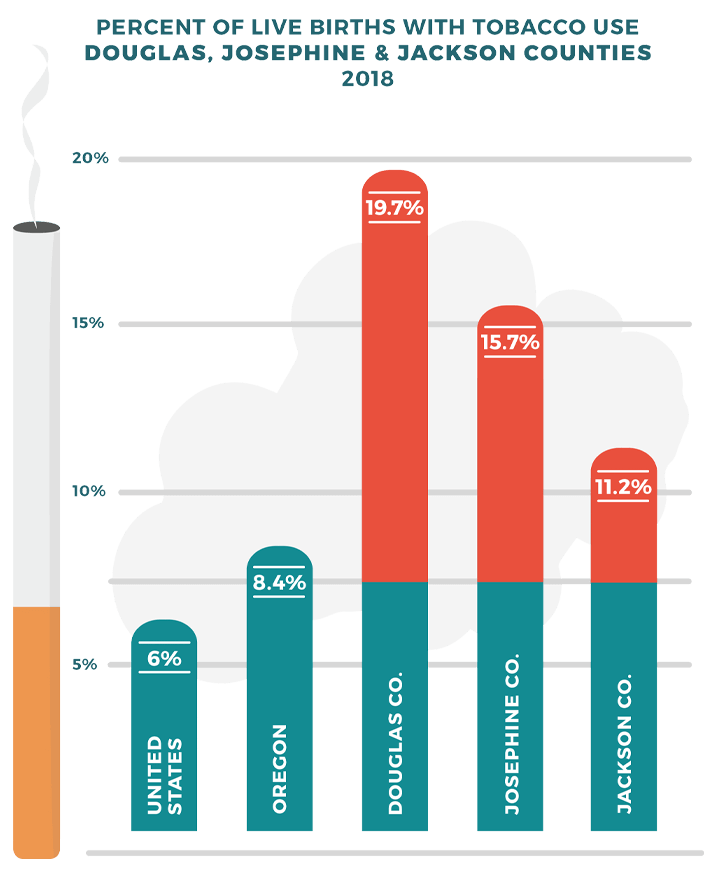
Maternal Smoking
Our region has alarmingly high rates of maternal tobacco use, with over 20% of women smoking during pregnancy — 31.5% in Douglas county and 38.3% in Josephine county in 2021. Women who smoke when pregnant have a far higher incidence of low birthweight babies than do nonsmokers. Smoking during pregnancy has also been linked with the following health risks:
- Problems with the placenta
- Premature birth
- Birth defects
- Low birth weight
- Pregnancy loss
Smoking during pregnancy can also increase the risk of sudden infant death syndrome (SIDS), colic, asthma, and childhood obesity.
How Do We Know About These Numbers?
Our program gathers important information about community health trends through our participants, and we use this information to help inform decisions about the program’s services. We also share this data with other stakeholders to help support efforts aimed at improving health outcomes. This data is anonymous, so no personal information is included.
Different types of data are gathered by our team. Our Data Analyst addresses our client-level data and has been with our program since the very beginning. Our Independent Evaluator has been connected to the program since 2012 and helps us explore community-level health trends and data.
Why Do We Collect Data?
“The data piece of the grant is very important. The numbers illustrate the impact we are making within the community we serve, not just in lowering infant mortality, but also looking at correlations between miscarriages, low birth weight or preterm deliveries and substance use or depression or domestic violence, or many other risk factors. This data is also taken to Congress to secure funding to do this important work.”
– Debi Michtom, Healthy Start Data Analyst

What Does This Mean for Southern Oregon?
While we are proud to be Healthy Start grantees and serve our local families, being a long-time grantee also means that Southern Oregon has been home to higher than average infant mortality rates and there are many aspects of our region’s health that need to be improved.
Just as the national infant and maternal mortality rates are higher for communities of color, our region reflects the same racial and ethnic disparities. Our community members who identify as racial and ethnic minorities are at higher risk for poorer infant and maternal health outcomes.
If you’re interested in seeing some of our region’s data, you can explore comprehensive reports from our independent evaluator.

How is Healthy Start Making an Impact?
As a program, we look at many different social determinants of health to gain a better understanding of the trends in our region that are impacting the health and well-being of women, infants, and their families.
The information in our Welcome Baby Resources are all tied to aspects of infant and maternal health that have big impacts on improving health disparities and represent goals of the Healthy Start program, including:
- Insurance, Well Visits, and other preventative care
- Family Planning
- Parent Education
- Infant Safety
- Mental Health & Substance Use Treatment
- Child Development
And because we are constantly gathering important data related to our program goals, we are able to see the impacts of the Healthy Start program on the families we serve throughout Southern Oregon.
Over 90% of Healthy Start clients have a primary care provider as their “medical home”
100% of Health Start clients receive a depression screening and referral for support as needed
92% of Healthy Start mothers initiate breastfeeding
Over 90% of Healthy Start infants are on schedule for well-baby visits and recommended vaccines
Want to Learn More?
Learn more about the federal program.
Curious about where these programs are across the country? Check out the Grantee map.
If you are interested in learning more about Infant Mortality Rates, including some of the causes and differences between populations, the CDC’s website will help you learn more.
Oregon by the Numbers is an outgrowth of an online tool (oregonexplorer.info/rural) that helps leaders explore data and statistics about their own communities. In order to serve the needs of Oregon, we need to understand the reality of what is happening across all of our communities. Numbers expose needs. Numbers reveal trends. Numbers track progress. Numbers identify successes. Through data collection and analysis, we can all make better decisions to promote the vitality and livability of Oregon. They help us understand where we need to look, listen and act to make positive differences in our communities.
Health Resources & Services Administration Statement
This web page is supported by the Health Resources and Services Administration (HRSA) of the U.S. Department of Health and Human Services (HHS) as part of an annual award totaling $1,100,000+. The contents are those of the author(s) and do not necessarily represent the official of, nor an endorsement by HRSA, HHS, or the U.S. Government.
